Here’s what you’ll learn when you read this post:
-
Cold atmospheric plasma is a real dermatology field, but “bio-harmonic” language is marketing rather than a recognized scientific term.
-
The strongest support so far involves acne, antimicrobial effects, and early facial rejuvenation findings, not dramatic one-session transformation claims.
-
Patients should ask for the exact device name, treatment category, and realistic outcome expectations before booking.
Why this treatment is getting attention
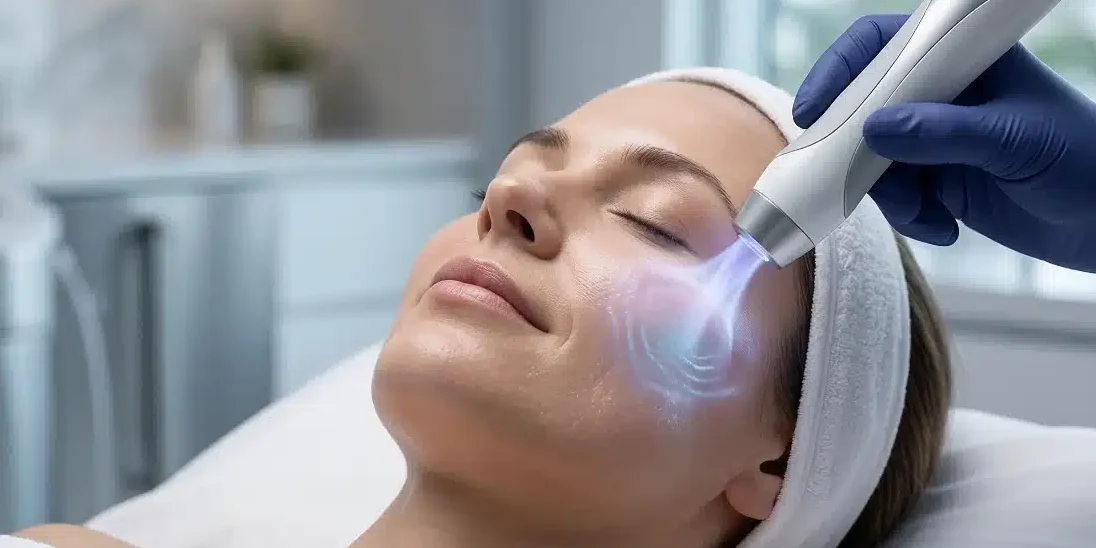
People often encounter this topic through polished imagery, calm clinical language, and promises of a gentler path to brighter-looking skin. The problem starts when branding runs ahead of evidence, because the phrase “bio-harmonic cold plasma” does not appear to be a standard scientific term in the reliable dermatology literature. The recognized medical term is cold atmospheric plasma, often shortened to CAP, and that distinction matters when someone tries to judge whether a treatment claim sounds credible.
A reader with persistent acne, surface dullness, or early texture changes may find the concept appealing for understandable reasons. Many people want something that sounds less aggressive than a resurfacing laser and more targeted than a vague facial. The evidence does support real medical interest in cold atmospheric plasma, but it supports specific uses and measured outcomes rather than sweeping claims about instant age reversal, deep tightening, or “energy balancing.”
The most useful starting point is simple. CAP appears to be a legitimate dermatologic research area, but the evidence hierarchy is narrower than the marketing hierarchy. The strongest patient-facing discussion today is not whether the phrase sounds futuristic, but whether the exact device, treatment goal, protocol, and expected result all line up with published evidence.
What cold plasma actually means in medical literature
Why the medical name matters
Cold atmospheric plasma is a partially ionized gas that can operate at temperatures close to room temperature, which is why researchers have explored it for skin-related use rather than treating it as a high-heat process. Reviews describe CAP as a technology that can generate reactive oxygen and nitrogen species along with other physical effects, and that combination helps explain why investigators keep studying it in dermatology. The term itself does not guarantee a cosmetic result, but it does point to a real field of research with defined mechanisms and growing clinical interest.
The name also protects patients from a common mistake: treating every device with “plasma” in the label as interchangeable. FDA guidance shows that Renuvion/J-Plasma uses radiofrequency energy and helium to generate plasma, and that different handpieces have different intended uses and limitations. That means a reader should never assume that a claim about one plasma system automatically applies to another, especially when the treatment goal is wrinkle reduction or skin tightening.
That distinction matters more in aesthetics than many patients realize. One clinic may use the word plasma as a shorthand for a gentle skin-surface treatment, while another may be referring to a system with a different energy source, different tissue target, and different evidence base. A credible consultation should make the device identity obvious before any promise about results is discussed.
What a session may look and feel like
What treatment usually involves
The facial rejuvenation study most relevant here used full-face low-temperature plasma once weekly for five consecutive sessions in 40 women with mild-to-moderate facial aging. In that study, the skin was cleansed first, treatment lasted about 20-minute sessions, and participants were advised to avoid sunlight afterward while using ointment and sunscreen during recovery. That kind of setup gives readers a more realistic frame than vague promises of a “single revolutionary treatment,” because the better-quality cosmetic data here came from a treatment series rather than a one-off visit.
A practical scenario helps. Someone with mild cheek roughness, visible fatigue around the eyes, and reluctance to accept the downtime of a more aggressive procedure may be drawn to a session that feels shorter and more manageable. The available rejuvenation study supports that some patients returned home after treatment and that the approach was pitched as a faster return-to-activity option than ablative methods, but it still required a structured series and aftercare.
What not to overread from the immediate glow
It is easy to mistake a fresh post-treatment look for proof that the deeper cosmetic promise has already been delivered. Readers should separate short-term brightness, which can happen after many skin procedures, from measured improvements that researchers assess weeks later with wrinkle scales or instrument-based readings. In the facial rejuvenation study, improvement was evaluated at four and twelve weeks after treatment, not by a mirror check five minutes after a device touched the skin.
That is one of the most important expectation checks in this category. A polished same-day photo can capture surface freshness, better lighting, or short-lived post-treatment change, yet it does not prove collagen remodeling, durable acne improvement, or visible tightening. Patients usually make better decisions when they ask how outcomes were measured and over what timeline.
Where the evidence looks strongest today
Acne has the clearest practical signal
If a reader wants the most defensible skin-focused use case, mild inflammatory acne currently has the clearest practical signal among the sources reviewed here. A 2025 randomized, controlled, double-blind pilot study enrolled 40 participants, gave both groups daily adapalene and weekly physician skin cleansing, and added either active CAP or placebo-device treatment. The CAP group showed stronger improvement in acne-specific investigator scores and other measured outcomes, while adverse events were less frequent and no serious adverse events were reported overall.
That result does not mean CAP has become a universal acne answer. It does mean a reader with mild papules and pustules, especially someone frustrated by irritation or by the limits of routine topicals alone, can discuss CAP as an add-on option with more confidence than someone seeking a broad anti-aging miracle. The same study still described itself as a pilot trial and pointed to the need for longer treatment periods and larger cohorts, so the most honest takeaway is “promising adjunct,” not “settled standard.”
Facial rejuvenation data are encouraging but still limited
The best direct cosmetic study in the current source set involved 40 women who received five full-face low-temperature plasma treatments. Investigators reported statistically significant improvement in wrinkle scores at four and twelve weeks, along with changes in melanin, erythema, and elasticity measurements in measured facial areas. Those are meaningful signals, yet the study design was a prospective cohort rather than a sham-controlled cosmetic trial, so the findings support cautious interest rather than overconfident promises.
This is where patient expectations often go off track. A person hoping to soften mild roughness, look less dull, or see gradual refinement in fine surface changes may be evaluating the treatment reasonably. A person expecting one session to lift lax skin, erase etched lines, and replace more established rejuvenation methods is stepping beyond what these sources can support.
The cleanest way to read the evidence is by treatment goal. Current support looks stronger for gradual improvement in mild surface concerns than for dramatic restructuring of deeper aging changes. That makes CAP easier to discuss as a limited, targeted option than as a wholesale substitute for every other rejuvenation category.
Why researchers keep studying it beyond cosmetics
Cold atmospheric plasma did not gain attention only because of aesthetic marketing. It is a real dermatologic research field rather than a cosmetic slogan, and a systematic review identified 166 studies included across multiple applications. The broader dermatology literature shows interest in microbial control, and one systematic review found that wound healing and melanoma treatment were the largest focus areas in the dermatology literature it analyzed.
Readers often hear broad claims about cold plasma skin technology, yet the underlying evidence comes from different kinds of studies with different goals. This quick-reference table helps separate where current research looks more practical, where it still looks early, and what that means for someone trying to make an informed decision.
| Evidence Area | What Researchers Studied | Typical Treatment Pattern in the Source Material | What Was Measured | What Readers Should Take From It |
|---|---|---|---|---|
| Mild inflammatory acne | A randomized, controlled, double-blind pilot study looked at cold atmospheric plasma as an add-on to standard topical care. | Weekly treatment sessions over several weeks, paired with cleansing and adapalene in both groups. | Investigator acne scores, lesion-related outcomes, and adverse events. | This is the most practical evidence area in the current source set, but it still supports an adjunct discussion rather than a universal acne solution. |
| Facial rejuvenation | A prospective clinical study evaluated low-temperature plasma for mild-to-moderate facial aging. | Five full-face sessions, usually performed once weekly, with aftercare that included sunscreen and sun avoidance. | Wrinkle scores, melanin index, erythema index, and elasticity-related measurements. | The results are encouraging for gradual cosmetic improvement, but the evidence does not support dramatic one-session transformation claims. |
| Microbial balance on skin | Recent research examined how plasma exposure affected microbial load and microbiome balance. | Controlled treatment conditions rather than a consumer-style cosmetic session comparison. | Sterilization effects and shifts in microbial balance. | This helps explain why acne and skin-surface hygiene claims sound plausible, although microbiome findings do not automatically prove a broad rejuvenation benefit. |
| Skin barrier tolerance | Human tolerance data assessed whether plasma exposure disrupted normal skin barrier function. | Short treatment exposures under controlled settings. | Barrier integrity and skin moisture. | The available safety signal is reassuring, yet it should be read as supportive evidence rather than proof that every plasma-labeled device behaves the same way. |
| Inflammation-related effects | Experimental work has explored anti-inflammatory effects in skin-related models. | Device-specific laboratory or early translational settings rather than broad cosmetic practice. | Markers tied to irritation, inflammation, or tissue response. | These findings help explain research interest, although lab signals should not be confused with guaranteed visible cosmetic outcomes for patients. |
| Wound-related applications | Review literature discusses CAP in wound healing and related dermatologic care contexts. | Protocols vary, which makes one-size-fits-all conclusions difficult. | Healing-related endpoints, antimicrobial effects, and tissue response. | This category shows that cold plasma has broader medical relevance, but wound-care evidence should not be stretched into blanket facial rejuvenation promises. |
| Device-specific limits | FDA material shows that plasma-based devices differ by energy source, tissue target, handpiece, and cleared indication. | Use patterns depend on the exact system rather than on the broad word “plasma.” | Regulatory indication, intended tissue level, and device category. | Readers should ask for the full device name before judging claims, because evidence for one plasma system does not automatically transfer to another. |
A practical way to judge the pitch before you book
Match the device to the claim
The first filter is not whether the treatment name sounds advanced. The first filter is whether the exact device being used has evidence that fits the exact claim being made. If the consultation cannot move quickly from branding language to a specific system name, that is a signal to slow down.
Match the goal to the published outcome
A second filter is treatment goal. The published material here gives more support for mild inflammatory acne as an adjunct discussion and for gradual refinement of mild facial aging than for dramatic lifting or replacement of established resurfacing categories. When a provider uses modest evidence to sell an oversized promise, the mismatch usually appears at this step.
Match the protocol to the promise
The better cosmetic data in this source set came from a series, not from a one-time event. That matters because a treatment that required five weekly sessions in a study should not be marketed as if one appointment typically delivers the same endpoint. Protocol details are not small print; they are part of the evidence.
Match the recovery plan to your actual skin behavior
Some patients care more about avoiding downtime than chasing the strongest possible endpoint. Others have reactive skin, pigment concerns after irritation, or a history of poor healing and need a more cautious strategy. A recommendation becomes more credible when it accounts for the person’s skin behavior instead of treating every face as the same canvas.
Safety questions and who should slow down
What the safety picture currently supports
The safety story looks encouraging, but it is not a blank check. Human tolerance data in the published literature support the idea that plasma treatment can be well tolerated without obvious disruption of normal skin barrier function, and broader reviews describe CAP as operating at room temperature with a favorable safety profile in many dermatologic contexts. Those points support cautious optimism, especially for readers comparing CAP with treatments known for more visible downtime.
At the same time, the current reviews explicitly say more research is needed to standardize duration, frequency, dosage, and broader clinical use. That limitation matters in real life because “cold plasma” describes a category, not a single universal protocol that every clinic applies the same way. A patient with highly reactive skin, pigment concerns after irritation, or a history of poor healing should treat the consultation as a decision point rather than a simple booking form.
Why device confusion can create unnecessary risk
A second safety issue is conceptual rather than physical: patients may hear “plasma” and assume the same evidence supports every device. The FDA’s Renuvion/J-Plasma communication shows that one plasma-based system uses radiofrequency energy and helium to generate plasma and that clearances differ by handpiece and intended use. A reader should therefore ask for the exact device name and treatment category before accepting any claim about tightening, resurfacing, or wrinkle reduction.
That question becomes even more important when marketing images show a sleek wand, a visible arc, and instant radiance. Those visuals can be effective, yet they do not tell a patient whether the treatment uses cold atmospheric plasma, another plasma-based system, or a device with very different evidence behind it. Staff at Fountain of Youth in Fort Myers, Florida stay current on developments in skin technologies like this, which matters because up-to-date device knowledge is often more valuable than dramatic wording on a menu.
What to settle before booking a consultation
A useful consultation should answer four practical questions without evasive language. The provider should name the device, explain the skin issue being targeted, describe what improvement would realistically look like, and tell you what alternative option would make more sense if this treatment is not the best fit. A conversation that jumps straight from “innovative plasma” to “you will love your glow” has skipped the parts that actually protect the patient.
A real-world example makes the difference clear. One reader may have mild acne with lingering redness and want a lower-intensity add-on discussion, while another may have deeper wrinkles and expect visible tightening after one session. The first scenario aligns better with the current evidence base, whereas the second needs a much more careful talk about limits, alternatives, and whether another category of treatment has stronger support for that goal.
A balanced consultation should also make it easy to walk away. When the recommendation is sound, the explanation usually stays specific, measured, and easy to compare against other options. When the pitch depends on mystique, urgency, or vague claims about energy and regeneration, the information quality usually drops fast.
Questions? We are here to help! Call 239-355-3294.
3 Practical Tips
Ask for the exact device name, not just the word plasma. That one step can prevent confusion between CAP-based treatments and very different systems with other energy sources, other tissue targets, and other FDA-cleared uses. A trustworthy answer should sound specific, not theatrical.
Ask how success will be measured for your specific concern. In the better studies, investigators tracked wrinkle scores, lesion counts, melanin index, erythema index, elasticity, or acne-specific assessments rather than relying only on compliments or post-treatment photos. Patients deserve that same standard of clarity in a real consultation.
Ask what the provider would recommend if this treatment were unavailable. That question lowers the marketing pressure and often reveals whether CAP is being chosen because it fits the problem or because it is the newest item on a service list. The conversation usually becomes much more useful once the answer includes a balanced explanation of limits as well as potential benefits.
FAQ
Is cold plasma the same as a plasma pen?
No. The current sources support cold atmospheric plasma as a real dermatologic research category, but FDA materials show that plasma-based devices can differ sharply in energy source, handpiece, tissue target, and cleared use. A patient should not assume that two treatments with “plasma” in the name share the same evidence or the same safety profile.
Is cold plasma treatment safe for facial skin?
The available evidence is encouraging, not absolute. Human tolerance data and broader reviews support the idea that CAP can be well tolerated in dermatologic settings, but that does not prove every plasma-labeled device behaves the same way on every patient. Clinical decisions still depend on device type, settings, treatment goal, and individual skin behavior, so safety needs to be discussed case by case.
How soon can visible results appear?
That depends on what result a person expects. In the facial rejuvenation study, outcomes were formally assessed at four and twelve weeks after a five-session series, which is very different from expecting a single same-day transformation. A short-term fresh look may happen, but the more meaningful claims in the current evidence were measured over time rather than judged immediately after treatment.
How many sessions are usually discussed?
The strongest cosmetic study in these sources used five weekly sessions, and the acne pilot used weekly treatments with an endpoint at six weeks and follow-up at ten weeks. That pattern suggests readers should expect a series discussion rather than assume one visit answers the whole question. Anyone promised dramatic, lasting improvement after a single session should ask how that claim matches the published evidence.
Can cold atmospheric plasma replace lasers, radiofrequency, or other rejuvenation treatments?
The current source set does not support that kind of blanket replacement claim. The available evidence is more consistent with selective use for certain goals, especially mild inflammatory acne as an adjunct discussion and gradual improvement in some mild facial-aging measures. A provider who presents CAP as one option within a broader treatment conversation is usually giving a more evidence-matched recommendation than one who presents it as the answer to everything.
Medical review: Reviewed by Dr. Keith Lafferty MD, Fort Myers on April 8, 2026. Fact-checked against government and academic sources; see in-text citations. This page follows our Medical Review & Sourcing Policy and undergoes updates at least every six months.