Transcranial photobiomodulation, often shortened to tPBM, has moved quickly from research journals into wellness conversations. Patients now encounter claims ranging from sharper thinking to migraine relief, often presented with confident language and polished devices. Sorting what current science actually supports from what remains uncertain requires careful reading of recent human trials, not marketing summaries. This article explains what tPBM is, what the best available 2024–2026 evidence shows, and how patients can approach it with realistic expectations.
Why people are suddenly hearing about tPBM
Interest in tPBM has grown for several reasons that have little to do with proven outcomes. The technology sounds intuitive because it involves light rather than drugs, and early laboratory findings are easy to summarize in appealing ways. Media coverage often blends animal data, small pilot trials, and mechanistic theories into simplified claims that feel authoritative. Patients dealing with cognitive changes, poor sleep, low mood, or chronic migraine often encounter tPBM after exhausting conventional options, which raises expectations even further.
Another reason for the surge is device accessibility. Wearable headsets and in-clinic systems now look consumer-friendly and are marketed as noninvasive and low risk. That framing encourages people to assume benefits are established, even when clinical evidence remains mixed or limited to specific outcomes. Understanding the distinction between plausible mechanisms and demonstrated patient benefit is essential before deciding whether tPBM is worth personal time and expense.
What tPBM actually is in human research
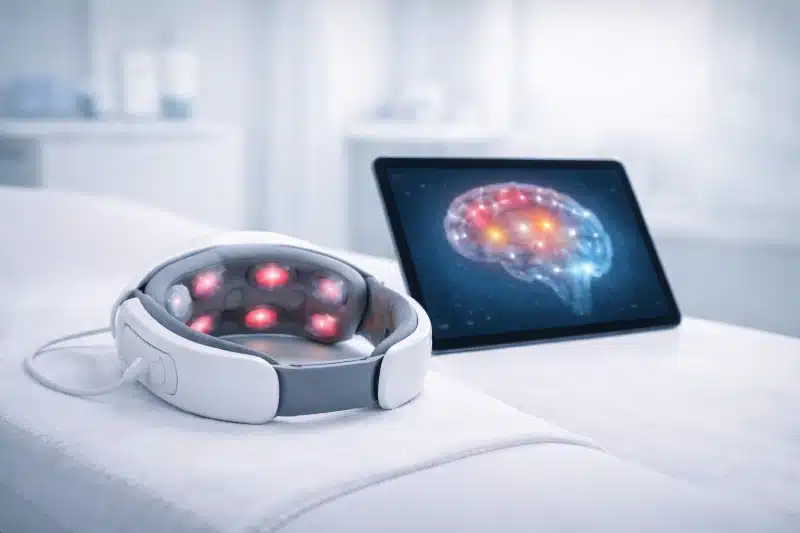
What tPBM actually is in human research
The basic idea in plain language
tPBM refers to delivering red or near-infrared light to the scalp with the intention of influencing brain function. In research settings, light in the 800–1,100 nanometer range is most commonly used. The light does not “shine through” the skull in a simple way; instead, a small portion penetrates superficial tissues and may affect underlying brain regions indirectly. Studies typically apply light for several minutes per session, repeated over days or weeks.
Researchers distinguish between transcranial approaches, where light is directed at specific scalp locations, and near-head approaches, where light is delivered more diffusely. Both fall under the tPBM umbrella in published trials, even though they may not produce identical biological effects.
Devices and setups you may see
Human trials have used several device types. Some rely on stationary clinical systems with arrays positioned over defined scalp regions. Others use wearable LED caps or headbands designed for home use under supervision. Differences in wavelength, power density, exposure time, and placement matter because they influence how much energy reaches target tissues. That variability explains why results from one study cannot be assumed to apply to every device marketed under the tPBM label.
What researchers measure to judge results
tPBM trials rarely rely on brain scans alone. Instead, researchers use cognitive tests, symptom questionnaires, sleep quality scales, headache frequency diaries, and standardized mood assessments. Safety outcomes are also tracked, including discomfort, headaches, or changes in vital signs. When reading claims, it helps to know whether outcomes were subjective, objectively tested, or both.
What scientists think might be happening in the brain
Several proposed mechanisms appear consistently across recent reviews. Light in the red and near-infrared range may interact with cellular components involved in energy production, particularly within mitochondria. This interaction is thought to influence cellular metabolism and signaling. Other hypotheses involve changes in cerebral blood flow and oxygen utilization, as well as modulation of inflammatory pathways.
Some studies also report changes in neurophysiological markers related to brain network activity. These findings suggest that tPBM could influence attention, arousal, or sleep regulation under certain conditions. Mechanistic signals, however, do not automatically translate into meaningful symptom improvement. Many interventions show biological effects without producing consistent clinical benefits, which explains why cautious interpretation remains necessary.
The evidence, separated by goal so claims stay honest
Cognition and mental performance
Cognition is the area where tPBM currently has the strongest human evidence base. A large 2025 umbrella review and meta-analysis pooling randomized controlled trials found statistically significant improvements across several cognitive domains, including global cognition, working memory, verbal memory, and executive function. These results indicate that measurable cognitive signals appear across studies when data are combined.
One placebo-controlled randomized trial in adults with mild cognitive impairment reported improvement in standardized cognitive scores and increases in a neurotrophic biomarker compared with placebo. Evidence for those points can be reviewed directly in the PubMed record for the randomized, double-blind, placebo-controlled trial reporting improved cognition and higher serum BDNF. Participants completed multiple sessions, and benefits persisted at short-term follow-up. These findings suggest that certain populations may experience modest cognitive gains under defined protocols.
Other human work has also connected cognitive performance to measurable brain-level changes. A related example appears in the PubMed entry describing an fNIRS study reporting working memory improvement and changes in functional brain networks in healthy older adults. Findings like these can help patients understand why researchers keep testing the approach, while still avoiding assumptions that every device or protocol will reproduce the same effects.
Limitations remain important. Trials vary widely in dose, schedule, and participant characteristics. Effects are not uniform across all individuals, and long-term durability beyond a few months remains unclear. Cognitive improvement in trials usually reflects small but measurable changes rather than dramatic restoration of memory or attention. Claims implying guaranteed or transformative cognitive effects exceed what current data support.
Mood, stress, and sleep
Mood outcomes are more nuanced. A 2025 randomized, double-blind, sham-controlled trial evaluating a wearable tPBM device in adults with major depressive disorder found improvement in both active and sham groups, without a significant difference between them for depression scales. That pattern suggests placebo effects and nonspecific factors play a substantial role.
Sleep quality outcomes from the same study differed. Participants receiving active tPBM showed greater improvement in sleep quality scores compared with sham. Evidence for sleep-specific benefit in controlled settings can also be examined in the PubMed listing for the randomized controlled trial in chronic insomnia reporting improved sleep quality and reduced daytime sleepiness. That type of outcome supports careful discussion of sleep as a potentially more responsive target than mood itself for certain low-burden protocols.
Patients should interpret mood-related claims carefully. Current evidence does not justify presenting tPBM as a stand-alone treatment for depression. Sleep improvements appear more defensible based on available data, especially when framed as supportive rather than curative.
Migraine and headache
Migraine represents the area where hype most clearly outpaces evidence. A systematic review of randomized trials evaluating photobiomodulation for primary headache disorders identified few studies and rated overall evidence quality as low. Although some trials reported pain improvements compared with sham, risk of bias and imprecision limited confidence in those findings.
The review concluded that existing evidence was insufficient to support photobiomodulation as a proven treatment for primary headache conditions, including migraine. This does not mean tPBM cannot help anyone with headaches, but it does mean claims of established efficacy are not supported by current high-quality data. Patients considering tPBM for migraine should view it as experimental rather than validated.
Below is a quick comparison of common tPBM parameters, what level of evidence exists for them in human studies, and typical expected experiences. This chart adds value by summarizing practical settings and evidence clarity that were not explored in depth above.
| Protocol Feature |
Typical Range in Studies |
Evidence Clarity Based on Published Human Trials |
What Patients Commonly Notice |
| Wavelength |
Near-infrared ranges commonly studied, including 808/810/1064 nm |
Used widely across cognition and mood/sleep studies, which supports comparisons within research settings |
Warmth at the scalp or no sensation at all |
| Dose and device variability |
Protocols vary by device type, placement, duration, and cumulative exposure |
Heterogeneity limits “one protocol fits all” claims, even when pooled results look positive |
Effects, if they occur, often appear gradually across sessions |
| Primary goal: cognition |
Global cognition, working memory, verbal memory, executive function |
Most consistently supported area in pooled randomized trial evidence |
Subtle functional changes, such as clearer focus or fewer “mental lapses” |
| Primary goal: depression |
Depression rating scales in controlled trials |
Between-group antidepressant benefit remains unclear in sham-controlled wearable settings |
Mood shifts may track with sleep changes or supportive care effects |
| Primary goal: sleep |
Sleep quality scores and daytime sleepiness measures |
Randomized trial evidence supports improved sleep outcomes in insomnia populations |
Faster sleep onset or fewer awakenings may be reported over time |
| Primary goal: migraine/headache |
Headache frequency, severity, disability, and rescue medication use |
Evidence remains low certainty, and existing trials do not justify “proven migraine therapy” claims |
Responses vary widely, and a clear predictable pattern is not established |
Who might consider tPBM, and who should be cautious
People most often represented in studies include adults with cognitive complaints, mild cognitive impairment, mood disorders under controlled conditions, and headache disorders in small trials. Individuals seeking incremental improvement rather than dramatic change tend to align better with current evidence.
Caution is appropriate for people with seizure disorders, implanted electronic devices, or complex neurological conditions. Pregnancy and unstable psychiatric illness also warrant clinician involvement before considering tPBM. Realistic goal-setting matters because disappointment often follows when experimental tools are treated as guaranteed solutions.
Ongoing research also matters for expectation-setting. A publicly accessible view of active and completed study designs is available through the ClinicalTrials.gov study record for a near-infrared transcranial photobiomodulation protocol. Listings like this help patients see how researchers define endpoints, duration, and safety monitoring in structured investigations.
What a session typically feels like
Most participants describe tPBM sessions as quiet and physically mild. Sensations may include warmth at the scalp or no noticeable feeling at all. Lack of sensation does not indicate lack of effect, just as sensation does not guarantee benefit. Immediate changes are uncommon; reported improvements typically emerge gradually over repeated sessions. Understanding this helps patients avoid premature conclusions based on a single visit.
Safety and side effects: what patients should know
Published safety analyses report mostly mild and transient effects, such as temporary scalp discomfort or headache. Controlled studies did not identify significant changes in weight or blood pressure across tested doses. Safety depends on dose, placement, and frequency, which is why responsible protocols matter.
Marketing materials sometimes omit discussion of dose parameters and monitoring. In research settings, participants are screened, informed of uncertainties, and followed for adverse effects. Patients should expect similar care standards when considering tPBM outside trials.
How to tell science-aligned care from trend-driven selling
Responsible providers can explain why a particular protocol is used, how progress will be measured, and when reevaluation will occur. They acknowledge uncertainty and avoid language promising cures. Trend-driven selling often relies on broad claims, testimonials without context, and explanations that jump from laboratory mechanisms to clinical certainty. Asking clear questions about goals, tracking, and stop points helps patients protect themselves from exaggerated expectations.
3 Practical Tips
- Set one clear goal before starting, such as improved sleep quality or better concentration, and track it consistently for several weeks.
- Ask for a written plan describing session frequency, target areas, and how response will be evaluated.
- Keep other lifestyle factors stable during a trial period so changes can be interpreted more accurately.
FAQ
Can tPBM improve memory or focus in healthy adults?
Current evidence suggests small cognitive benefits may occur in some adults, particularly when data are pooled across studies. Effects tend to be modest rather than transformative, and not everyone responds. Long-term durability remains uncertain.
If sleep improves, does that mean depression will improve too?
Sleep improvement does not automatically translate into antidepressant effects. A recent sham-controlled trial showed better sleep outcomes with active tPBM while depression scores improved similarly in both active and sham groups.
Is tPBM a proven migraine treatment or still experimental?
Based on available randomized trials and systematic reviews, tPBM remains experimental for migraine. Evidence quality is low, and claims of proven effectiveness are not supported.
How many sessions does it usually take before people notice anything?
Studies typically involve multiple sessions over several weeks. Immediate changes are uncommon, and any benefit usually appears gradually, making short trials difficult to interpret.
What “success” looks like when expectations are grounded
Success with tPBM often means small, measurable changes that improve daily functioning rather than dramatic symptom resolution. Better sleep quality, slightly improved attention, or subtle cognitive gains may matter when accumulated over time. Clear baselines and predefined evaluation points help patients decide whether continued use makes sense.
Fountain of Youth in Fort Myers keeps staff current on developments related to tPBM so patient conversations stay evidence-grounded and practical.
Questions? We are here to help! Call 239-355-3294.
Medical review: Reviewed by Dr. Keith Lafferty MD, Medical Director at Fountain of Youth SWFL on February 5, 2026. Fact-checked against government and academic sources; see in-text citations. This page follows our Medical Review & Sourcing Policy and undergoes updates at least every six months. Last updated February 5, 2026.




